Share
|
Getting your Trinity Audio player ready...
|
Children in Fresno and elsewhere in California face long wait times to get mental health care. In fact, a November report from the California State Auditor’s office shows that wait times for appointments sometimes reach as long as 100 days.
Moreover, a lack of oversight by governing agencies obscures how bad the problem might be.
Behavioral health providers say that with the changes to Medi-Cal reimbursement rates, those problems may be compounded as providers retreat from counties. As bigger contractors pick up where struggling health providers cannot, the auditor’s office casts doubt on their ability to cover those services.
“(The Department of Health Care Services) must make improvements to the way it monitors the capacity of Medi-Cal managed care plans to provide services for their members,” the report stated. “For example, DHCS approves potentially unreasonable standards for the time and distance Medi-Cal members must travel to see behavioral health care providers. Furthermore, the department’s enforcement activities do not always ensure that a plan takes steps to meaningfully improve access.”
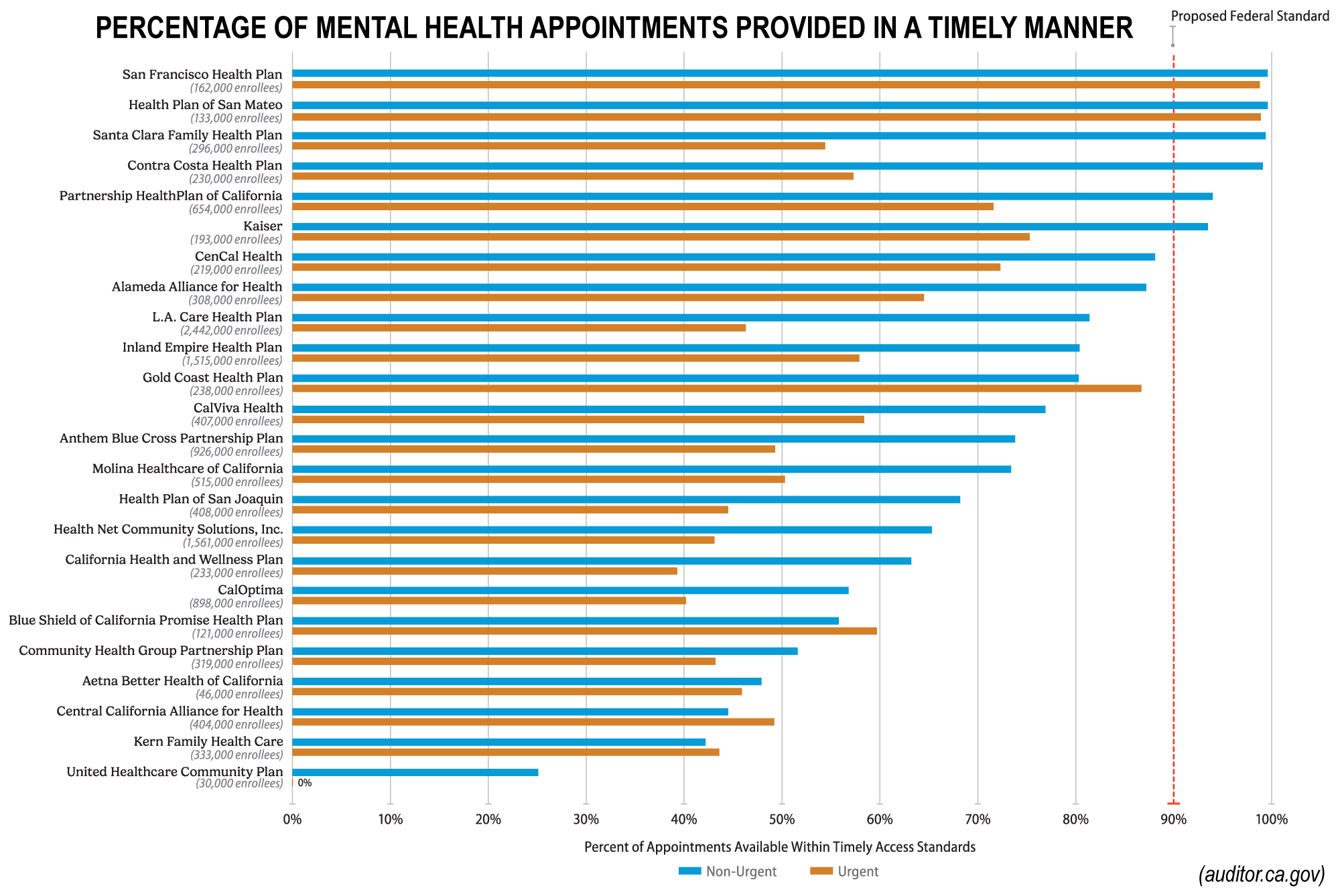
The auditor’s office reported in November that only 63% of therapists surveyed could provide an appointment time within the state’s mandated 10-business day standard for non-urgent appointments.
Urgent appointments were even harder to get with only 39% of therapists able to schedule an appointment in the maximum 96 hours. The median wait time for emergency mental health care reached almost 13 days.
But this data is from 2021 and 2022. And, since then, the state has changed the way it reimburses behavioral health providers. Providers say that reductions in payments from their respective counties have them seriously reviewing what services they can provide.
1 in 5 Teens Report Mental Health Challenges
Nearly 1 in 5 children between 12 and 17 years old report having had a major depressive episode, according to the U.S. Centers for Disease Control and Prevention.
One in three high school students in 2019 reported feeling sad or hopeless. Nearly 1 in 5 said they have seriously considered attempting suicide.
At the least, these challenges affect the way children learn, behave, and handle their emotions.
Suicide is the second leading cause of death for children and young adults between 10 and 14 years old, according to the CDC.
California Mandates Quick Access to Care. It Isn’t Happening.
In California, Medi-Cal covers 5.7 million children. But for those children needing care, the auditor’s office found children having to wait extended periods before seeing a mental health professional.
The state requires that urgent appointments be available within 48 hours for services that don’t need prior authorization. Urgent appointments that need authorization shouldn’t take longer than 96 hours, according to state law. Non-urgent appointments should be available within 10 business days and appointments with specialist physicians, including psychiatrists, should be available within 15 business days.
Only six healthcare plans could provide mental health appointments for non-urgent needs within the proposed federal standard for wait times. Only two providers could schedule appointments within the proposed federal standard for urgent needs.
To review wait times for children, the auditor’s office had to rely on surveys conducted by the DHCS and the Department of Managed Health Care, both of which oversee the administration of many behavioral health programs.
The auditor prefaced the study by saying those surveys were lacking.
“We found that neither DHCS nor Managed Health Care collect statewide data about how long patients wait for requested appointments and instead monitor timely access by other means,” the report stated.
DHCS says it does not have the software necessary to track that information.
California is among many states that don’t have a clear picture of wait times. Twelve other states the auditor’s office reviewed did not track wait times.
The auditor had to rely on surveys conducted by DHCS. Of those surveys, roughly two-thirds of the Medi-Cal providers in the survey were excluded from the calculation of wait times, said Adrienne Shilton, vice president of public policy and strategy with the California Alliance of Child and Family Services.
Based on those surveys, the median appointment wait time statewide was three days. But when appointments were delayed, they were severely delayed.
The survey found 26% of non-urgent appointments exceeded the 10-day standard. When it was exceeded, the median wait time was 23 days. Some took 100 days or longer. For urgent appointment needs, 43% of urgent appointments exceeded the 96-hour standard. The median wait time for those delayed appointments reached 13 days.
Fresno County Doesn’t Meet State Minimums for Appointments
Differences in completeness and accuracy of county-level wait-time data made comparing counties difficult, according to the auditor’s office.
One shortfall in the DHCS survey came in Fresno County, where by combining wait times for adults and children, DHCS showed that Fresno County was in compliance.
However, if the county had separated wait times for adults from children, it would have showed 76% of appointments for children meeting mandatory maximums, 12 percentage points lower than adults, and not in compliance with state mandates.

New Medi-Cal Payment System Threatens Services
To decrease wait times, Medicare standards dictate that counties hire enough providers. However, a new payment initiative has providers pulling back services statewide.
In July 2023, California rolled out its new reimbursement model to its behavioral health contractors.
The amount reimbursed to providers varies county-by-county. Providers were told they would only get a fraction of what they used to get.
Providers are now assessing what they can do, said Marilyn Sliney, regional executive director for Pacific Clinics in Fresno. Sliney said the network could be compromised, losing the resources it needs to help patients.
“We as an agency and we all as providers are having to determine if the rates received make it possible for us to continue providing the care that we’re providing,” Sliney said.
Some behavioral health providers reported seven-figure reductions in payments.
“If providers have to reduce community/field-based services, and/or reduce programming, access to care problems will only be compounded,” Shilton said.
Audit Casts Doubt on Whether Large Providers Can Cover the Gaps
The reduction in payments has led to a greater reliance on larger providers — defined as those with coverage in more than one region. Already, multi-county providers are having to pick up where smaller providers can’t.
One representative from Star Behavioral Health — a multi-county provider — said it is picking up contracts from providers that have closed or returned contracts to the counties.
But the auditor’s office found larger providers have been hesitant to see patients using Medi-Cal. The representative from Star said it hasn’t down Medi-Cal patients.
“Of the 16 providers we spoke to, nearly half expressed concerns related to providers’ willingness or ability to see members enrolled in Medi-Cal,” the report stated. “Three providers explained that they were currently not treating Medi-Cal patients or were transitioning away from doing so; all three cited low Medi-Cal compensation rates as a key factor.”
DHCS has relied on large providers to show compliance with provider-to-member ratios. DHCS’ calculations assume that larger providers spend all their time with Medi-Cal patients when, in fact, nearly half provided fewer than two services per month to children in Medi-Cal.
The more regions a provider covers, the more that DHCS overestimates its coverage. DHCS overestimated the capacity of providers covering two regions at four times their actual capacity. Those covering three regions were overestimated by six times.
Payment Reform Creates Barrier to Face-to-Face Counseling
The audit found that DHCS had set standards approving excessively far travel times to get to care facilities. In some cases, children in rural areas had to travel two or more hours for care.
California defines Fresno County as a “small county,” where a 75-minute trip or 45 miles to a facility is the maximum standard. Part of the back-and-forth involves therapists driving out to see clients. But under payment reform, travel time is no longer covered.
Therapists travel out to cities such as Orange Cove, Mendota, or Firebaugh.
While telehealth has become a useful tool, there are those who need in-person care, said Marilyn Sliney, regional executive director for Pacific Clinics.
“They need someone there to connect with them, to be with them, to provide their services in person in their communities and in their schools to help to be able to address the really complex needs,” Sliney said.
RELATED TOPICS:
Categories

Fresno Police Seek Missing 14-Year-Old Girl

Iran Threatens Painful Response if US Renews Attacks

Britney Spears Charged With One Misdemeanor in DUI Case